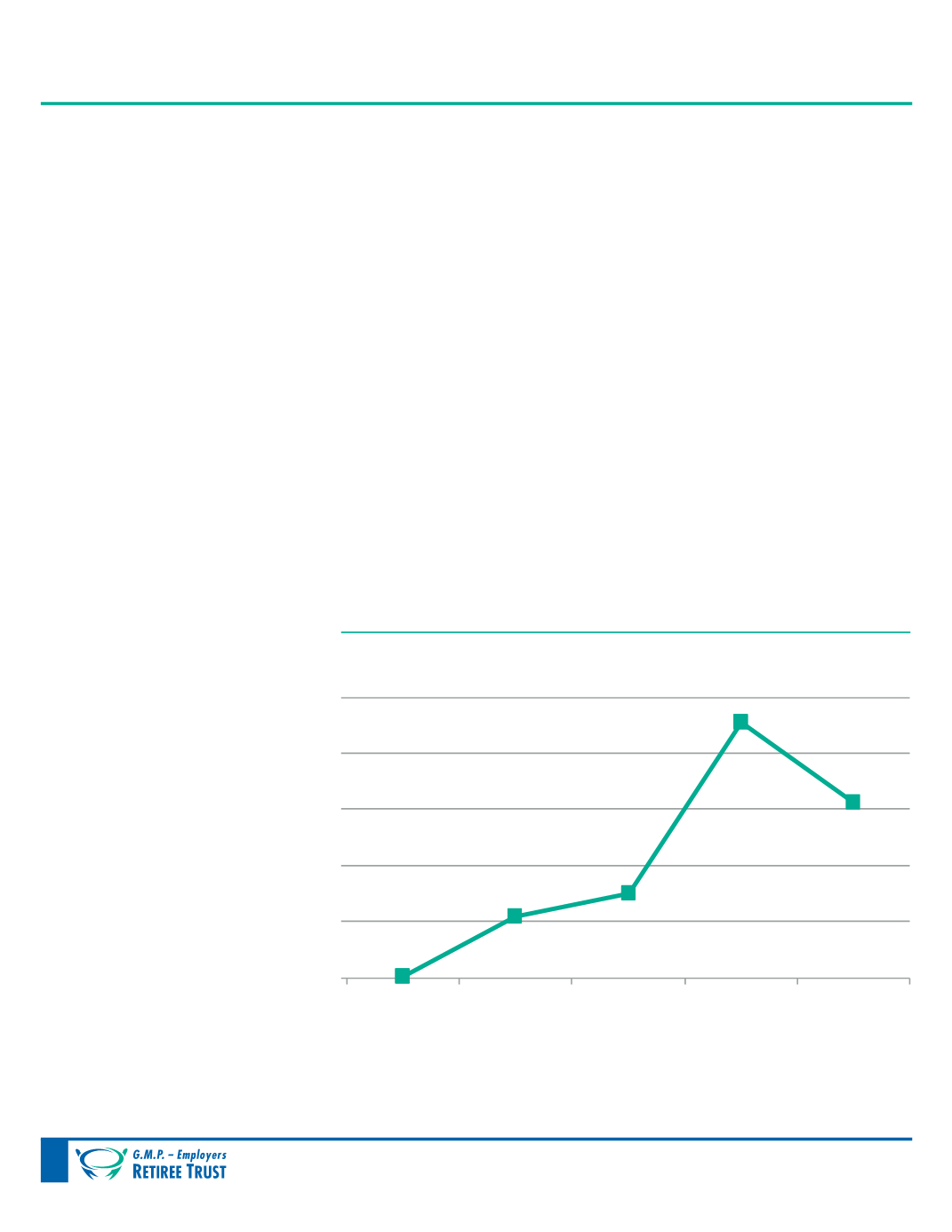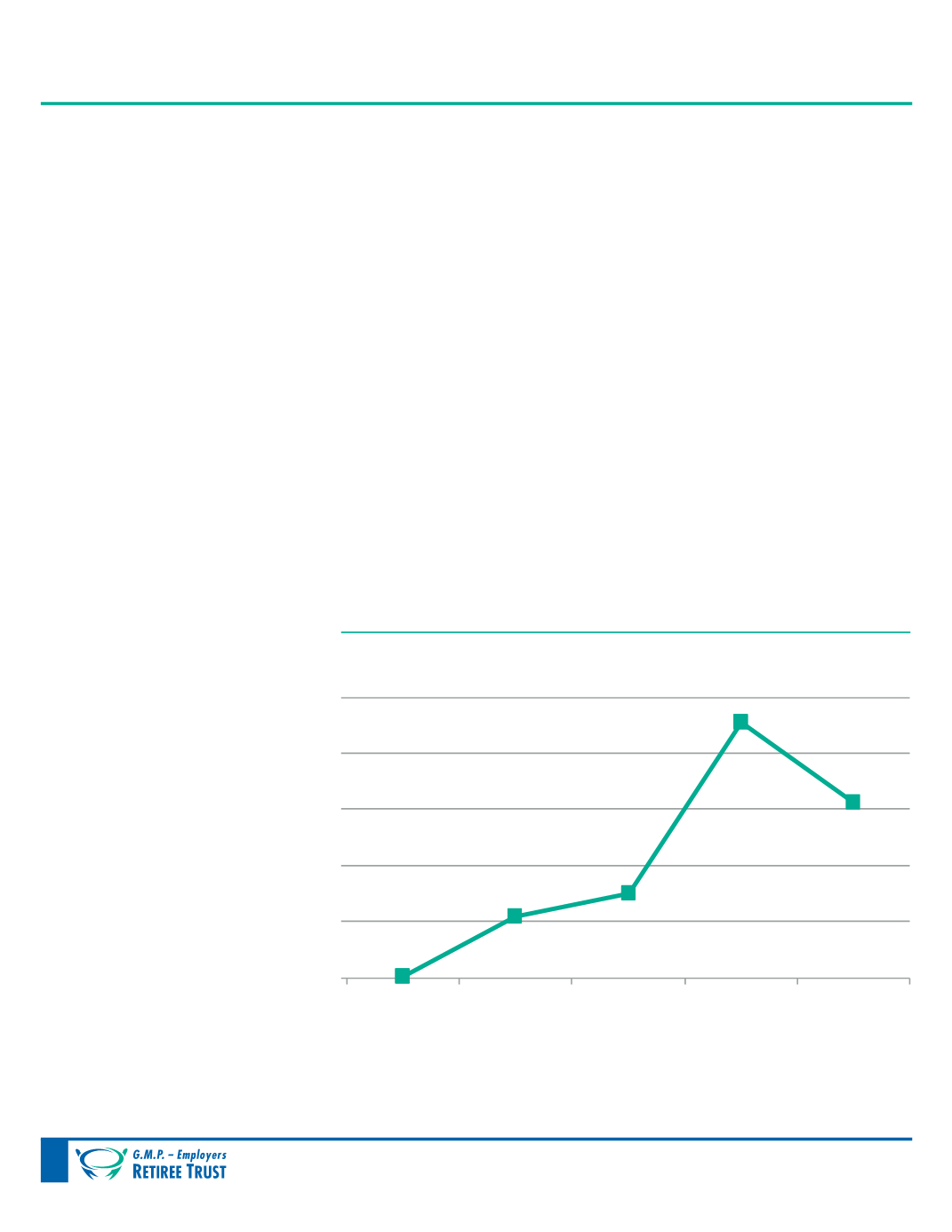
4
Factors Affecting the Trust
Claims Payment
Trends
As the graph below depicts,
claims payments by the Trust
increased steadily in the 1980s
and into the 1990s. After the
mid-1990s, the increase in claims
payments accelerated. This was
due, in part, to the elimination of
the age 60 eligibility requirement
in 2000, and the prescription drug
benefit the Trust made available
in January 2002. In 2015, the
overall net plan cost increased by
2.7%. Prescription drug claims
continue to be a growing share of
the Trust’s total costs. In 2015,
the prescription drug plan costs
net of rebates and subsidies was
$7.6 million, or 25.1% of medical
claim payments. Non-Medicare
eligible participants comprise
13.2% of total participants, but
approximately 48.3% of total
claims paid.
Prescription Drug
Coverage
In 2015, 88.8% of prescriptions
were for generic, and this rate
exceeds comparable plans by
5.5%. In addition, 98.3% of
participants have selected a
generic or preferred prescription
drug. The use of generics and
preferred prescription drugs
is a significant savings to the
participants and the Trust.
High-Cost
Specialty Drugs
High-Cost Specialty Drugs is
one element of pharmacy benefit
programs that continues to
grow at a much faster rate than
the rest. Specialty drugs, which
include biologics, injectables,
and other pharmaceutical
innovations, are no longer an
emerging category of pharmacy.
They are a fact of life and a
growing portion of overall
pharmacy benefit spending.
In 2015, the prescription plan cost
per member per month (PMPM)
trend on specialty drugs is 35.8%,
compared to a 0.4% plan cost
PMPM trend on non-specialty
drugs. The number of scripts for
specialty drugs decreased by 3.2%
in 2015, but the cost per script
increased 35.8%.
99,346
10,871,533
15,154,611
45,627,587
31,341,919
1967
1985
1995
2005
2015
Total Claims Paid
Claims Paid in 2015:
Medical = $30,181,919 Life = $1,160,000